Dental implants have revolutionized the field of dentistry, providing a reliable and aesthetically pleasing solution for individuals with missing teeth. However, like any medical procedure, complications can arise. Two common issues that can lead to dental implant failure are mucositis and peri-implantitis.
What is Mucositis?
Mucositis is a common inflammatory condition that affects the soft tissues surrounding dental implants. It occurs when bacteria accumulate around the implant site, causing inflammation of the mucous membrane. According to Dr. John Bruce of the Mugford Center for Periodontics and Dental Implants, “Poor oral hygiene, smoking, diabetes, and a weakened immune system can contribute to the development of mucositis.”
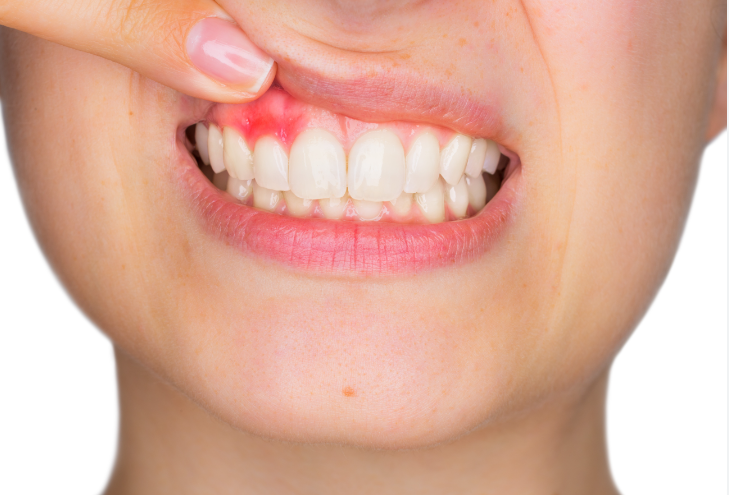
Symptoms of mucositis include redness, swelling, bleeding, and discomfort around the implant site. “If detected early,” says Dr. Bruce, “mucositis can be reversed and managed with proper oral hygiene practices, including regular brushing, flossing, and professional cleanings. However, if left untreated, mucositis can progress to a more severe condition known as peri-implantitis.”
Understanding Peri-implantitis
Peri-implantitis is a destructive inflammatory disease that affects the tissues surrounding dental implants, including the bone and gums. It is often considered the most common cause of dental implant failure. Peri-implantitis shares similarities with periodontal disease, as both involve bacterial infection and the subsequent destruction of supporting tissues.
When mucositis progresses to peri-implantitis, the inflammatory response leads to bone loss around the implant. This bone loss weakens the implant’s stability and can result in the eventual failure of the implant. Common risk factors for peri-implantitis include a history of periodontal disease, poor oral hygiene, smoking, diabetes, and genetic predisposition.
Symptoms of peri-implantitis include swelling, redness, bleeding, pain, gum recession, implant mobility, and the presence of pus. If left untreated, peri-implantitis can cause significant damage to the implant and surrounding structures, potentially leading to implant failure.
Prevention and Treatment
Preventing mucositis and peri-implantitis is crucial for the long-term success of dental implants. Here are some strategies to minimize the risk:
- Strict oral hygiene: Regular brushing, flossing, and interdental cleaning are essential to remove plaque and bacteria that can lead to infection. Interdental cleaning helps remove debris and interproximal dental plaque, the plaque that collects between two teeth.
- Professional cleanings: Regular visits to the Mugford Center for professional cleanings and check-ups are crucial for maintaining oral health and detecting any signs of mucositis or peri-implantitis early on.
- Smoking cessation: Smoking is a significant risk factor for both mucositis and peri-implantitis. Quitting smoking can significantly improve the chances of successful implant outcomes.
Health management: Maintaining a healthy lifestyle, managing conditions such as diabetes, and boosting the immune system can contribute to better implant health. - Regular monitoring: Patients should have dental professionals regularly monitor the health of dental implants and assess the condition of the surrounding tissues to identify any signs of inflammation or infection promptly.
The Mugford Center is uniquely qualified to treat peri-implantitis because of our extensive knowledge of multiple implant systems and the different etiologies which can contribute to the issue.
“We have invested hundreds of hours in continued education on understanding how to minimize the chance of peri-implant mucositis and peri-implantitis from the point of surgery, to the prosthetic design of the implant crown, to the technique and schedule for maintenance,” notes Dr. Bruce. “Further, and when needed, we have the ability to use the Erbium YAG laser to sterilize an exposed implant surface without damaging the micro-topography or heating the implant in a case of peri-implantitis. This gives us the best chance to help the patient regenerate bone and achieve health again.”
Summary
In the case of mucositis or early-stage peri-implantitis, non-surgical treatments may be effective in managing the condition. These can include professional cleanings, antimicrobial rinses, and local application of antibiotics. However, advanced cases of peri-implantitis may require more invasive treatments, such as the Erbium YAG laser, bone grafting, or implant removal.
To protect your investment in dental implants, we encourage you to contact our office so that we can have a look and create a strong mitigation and health program. Give us a call today to schedule your exam: (410) 260-0790.